Join Us At the 2026 NEI Spring Congress and Explore How Emerging Biomarkers and Biotypes are Shaping More Precise, Effective Care.

May 1-3, 2026 | Kissimmee, Florida
Featured Session: The Personal Touch: Utilizing Biotypes and Biomarkers in the Diagnosis and Management of Difficult-to-Treat Depression
Presented by Roger S. McIntyre, MD, FRCPC
View Agenda and Register
A new perspective by van Bruggen and McIntyre (2025) argues that inconsistent results in trials of anti-inflammatory and insulin-sensitizing treatments for major depressive disorder (MDD) and bipolar disorder (BD) may reflect biological heterogeneity—not lack of efficacy.
“The overarching aim of this paper,” Dr. Roger McIntyre explained, “is to propose metabolic and inflammatory biomarkers that could be considered as an approach to discovering and developing new treatments for bipolar and related disorders.”
Substantial evidence now links low-grade inflammation and insulin resistance (IR) to a meaningful subgroup of patients with mood disorders. In BD, 20–40% of patients show inflammatory abnormalities, and metabolic syndrome affects roughly one-third. In MDD, elevated CRP, IL-6, and TNF-a are reported in subsets of patients, while IR is associated with atypical symptoms, greater illness burden, and poorer antidepressant response.
Importantly, IR in BD is linked to worse cognitive performance, reduced hippocampal volume, more chronic illness course, and diminished response to mood stabilizers.
“We do believe that metabolism and inflammation are playing a role,” Dr. McIntyre noted. “Which then stands to reason that if you have a treatment that targets metabolism and/or inflammation, that might be most likely to be effective in someone who has metabolic or inflammatory markers.”
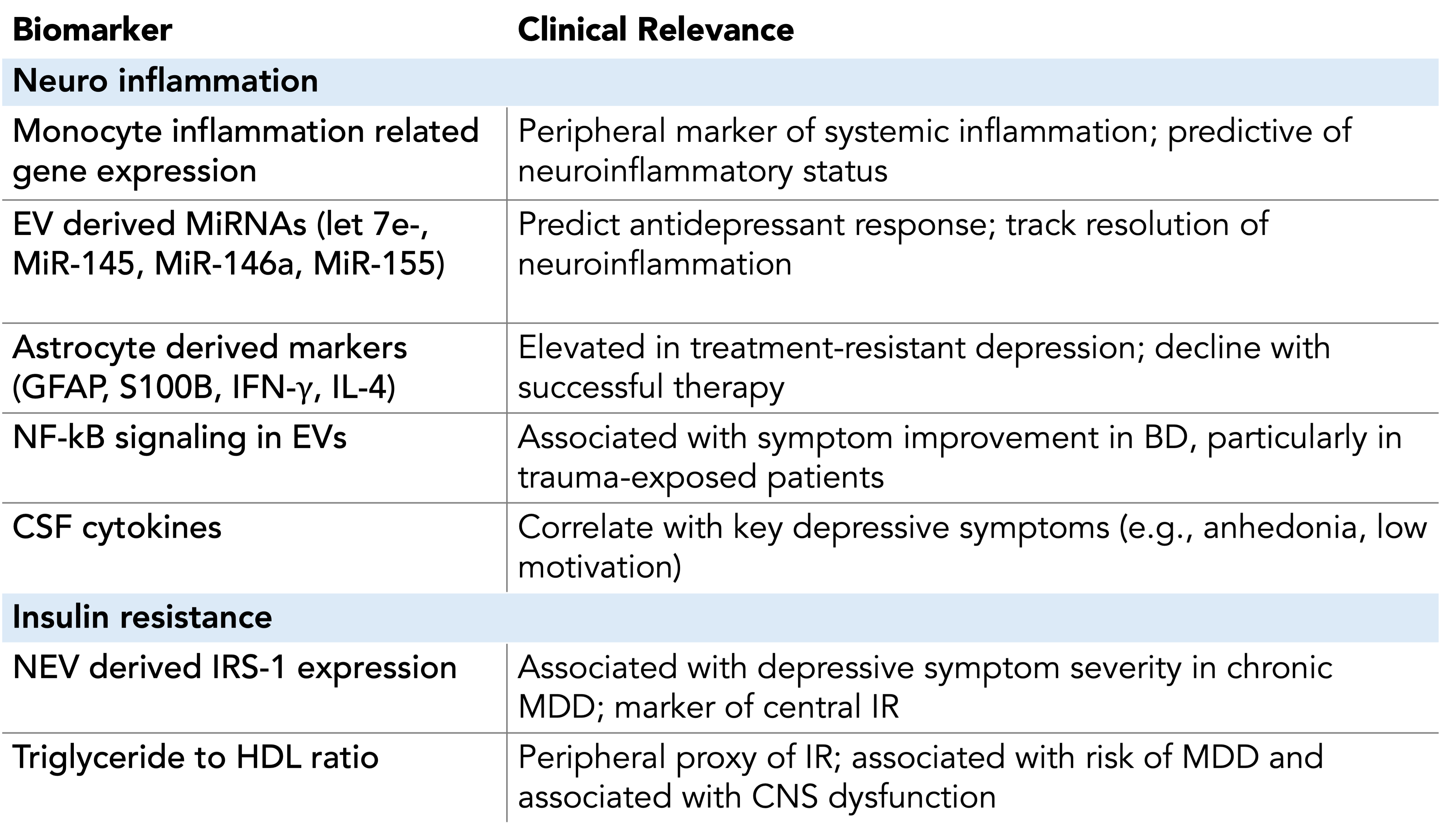
Summary of biomarkers relevant for identifying the immunometabolic phenotype in mood disorders.
Why Many Trials Appear “Negative”
Several immunometabolic interventions, such as fish oil, statins, anti-inflammatory agents, and insulin sensitizers, have shown modest or inconsistent effects in unselected samples.
“Fish oil and other anti-inflammatory treatments don’t have a very strong effect size in treating depression,” Dr. McIntyre said. “But when you enroll people on the basis of having an inflammatory problem, say, elevated C-reactive protein (CRP), and they have depression, that person might be more likely to benefit.”
Similarly, in treatment-resistant BD with confirmed insulin resistance, metformin has demonstrated clinically meaningful benefit, particularly when insulin sensitivity improves. The implication is not that these agents do not work, but that they may work best in biologically enriched populations.
“We believe if you select patients who meet DSM-5 criteria but also exhibit biological alterations in those markers, the drug is more likely to work,” he added.
Moving Beyond Single Markers: The Multimodal Approach
A key message of the paper is that no single biomarker—such as CRP—is likely to be sufficient.
Instead, the authors advocate for multimodal immunometabolic biosignatures, integrating:
- Inflammatory markers (e.g., cytokines, monocyte gene expression)
- Metabolic indices (e.g., HOMA-IR, TG/HDL ratio)
- Extracellular vesicle (EV) signatures reflecting central inflammation)
- Genetic and epigenetic features
- Clinical variables such as obesity, diabetes, hypertension, or trauma exposure
These combined datasets could then be analyzed using machine learning or other advanced analytic methods to identify biologically coherent subgroups most likely to benefit from targeted therapies.
“It kind of all hangs together in a way that I think is very logical and coherent,” Dr. McIntyre added. “Not everybody responds to a metabolic or inflammatory treatment—but people who have an alteration in those systems appear more likely to respond to interventions targeting those systems.”
Clinical Takeaways
For clinicians, the practical implications are becoming increasingly difficult to ignore:
- Routinely screen for metabolic dysfunction in patients with mood disorders..
- Consider insulin resistance in cases of treatment resistance, persistent cognitive impairment, or atypical illness trajectories.
- Recognize that a subset of depression and bipolar disorder may represent an immunometabolic phenotype—one that may require targeted metabolic intervention rather than repeated adjustments of psychotropic medications alone.
At the same time, caution is warranted. As Dr. McIntyre noted: “I often get asked whether we should check CRP or other inflammatory markers. I don’t think we should—not just yet. We still need to validate that. But metabolism for sure—we should be checking for insulin resistance and so on.”
In other words, while inflammatory biomarkers remain an area of active investigation, metabolic assessment is already clinically actionable.
This framework does not replace symptom-based diagnosis. Rather, it refines it. It offers a possible explanation for heterogeneity in treatment response, for cognitive variability, and for why certain therapies yield inconsistent results in large trials.
Rather than asking whether inflammation or insulin resistance matter in mood disorders, the more clinically useful question may be: are we identifying the patients in whom they matter most?
Reference:
van Bruggen FH, McIntyre RS. Brain Behav Immun Health. EHealth 2025;51:101166. Abstract
Join Us At the 2026 NEI Spring Congress and Explore How Emerging Biomarkers and Biotypes are Shaping More Precise, Effective Care.

May 1-3, 2026 | Kissimmee, Florida
Featured Session: The Personal Touch: Utilizing Biotypes and Biomarkers in the Diagnosis and Management of Difficult-to-Treat Depression
Presented by Roger S. McIntyre, MD, FRCPC
View Agenda and Register >
Additional education and resources:

Patient Education
Side Effects Diary
Worksheets and forms your patients can use to help gather and track their data.